Orly Shamir made Canadian medical history when she became the first person in the country to receive a bionic eye.
In a clinical trial six years ago, Dr. Robert Devenyi and his surgical team at a Toronto hospital implanted an Argus Retinal Prosthesis System (Argus II) onto the surface of Orly’s retina.
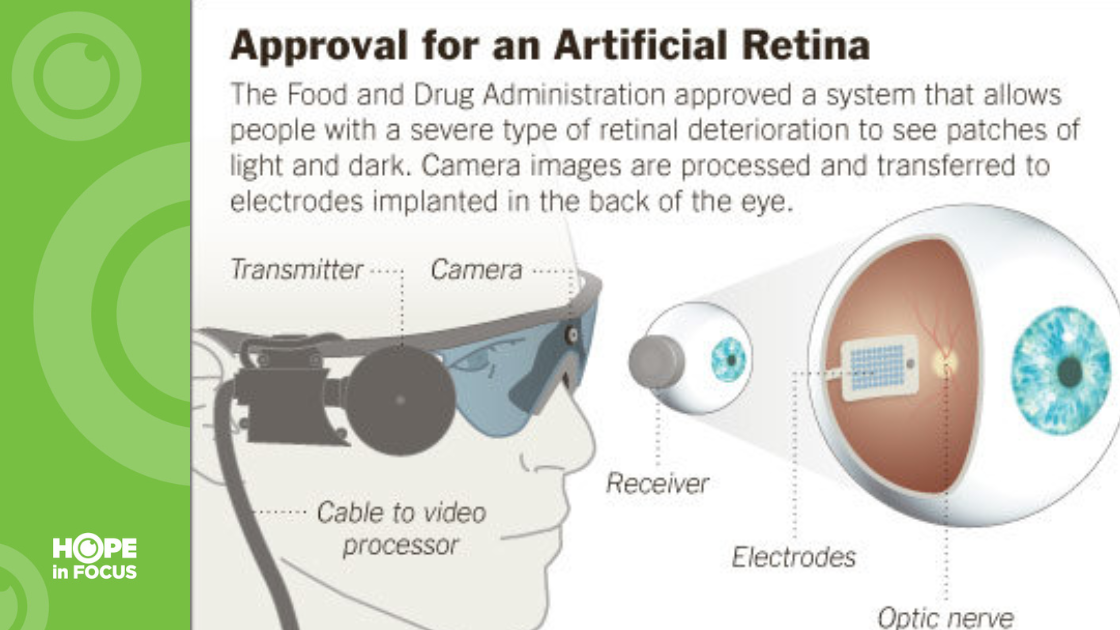
The Argus II, known as the bionic eye, stimulates the eye with electrodes to transmit visual information captured by a video camera to the patient’s brain. Toronto Western Hospital-University Health Network and Foundation Fighting Blindness provided support as collaborators on the 2014 clinical trial. California-based Second Sight developed the device.
Health Canada approved the system in 2015. It was approved in the United States in 2014 and in Europe in 2011.
Orly has a form of Leber congenital amaurosis called LCA4 caused by a mutation in her AIPL1 gene. She could read large print as a child, but her vision deteriorated to minimal light perception and shadows in her 20s. Now 52, Orly took part in the 2014 trial when she was 46.
Photoreceptors in a healthy retina convert light into electrochemical pulses sent through the optic nerve and into the brain where they are decoded into images. When photoreceptors don’t function properly, as in the case of people with LCA, the first step in the vision process is disrupted and cannot transform light into images.
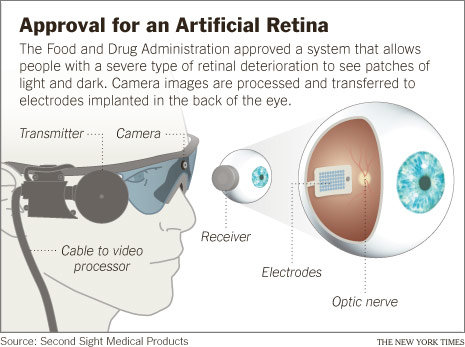
The Argus II bypasses damaged photoreceptors through electrodes implanted on the retina. Following the delicate three-hour surgery, Orly wore glasses containing a tiny camera that converted video images into a series of small electrical impulses transmitted wirelessly to the electrodes. Visual information transmits to the brain’s optic nerve when the pulses stimulate the retina’s remaining cells.
The visual improvement does not equal regular sight, but it allows patients to perceive light patterns, observe whether doors and windows are open, or pick up a glass.
Orly worked with rehabilitation experts, low-vision therapists and consultants from Second Sight. Three months following the surgery, she could detect contrast and recognize the difference between white and black. Because patients receive a form of artificial vision through this bionic eye, they need to re-train their brains through rehabilitation to learn and understand messages sent by the device. It’s kind of like learning a new language.
Orly volunteered to take part in the clinical trial for a year but presently does not use the technology.
“I worked hard for two years, then decided to not use the system for personal use, as it didn’t provide any benefits as of yet.”
Orly’s participation is exactly what a clinical trial is all about. She committed to making frequent visits and underwent testing over the course of a year. She knew that the goal of a clinical trial is to see whether a potential treatment is safe and effective, and that, while a trial participant might benefit, the trial’s purpose is to determine if the therapy works.
“I was prepared in being part of advancing technology for blind/visually impaired people in the future. That’s always who I am,” she said. “I’m 100 percent ready and available to get updates and keep trying.”